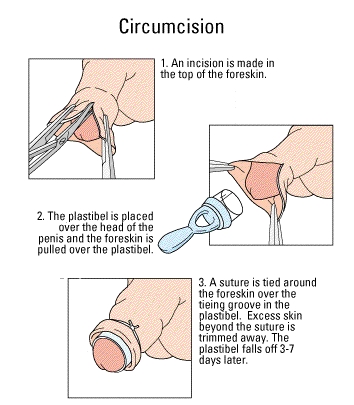
Plastibell
The Plastibell Circumcision Device is a clear plastic ring with a deep groove running circumferentially designed for circumcising infant males. It was invented by Hollister Inc in 1950, and first reported on in 1953.[1][2] The device works bo providing a circumferencial surface upon which to tie off the foreskin.
Advantages
The glans is protected during the procedure by the ring. Hemostasis (control of bleeding) is effective due to the ligature tie. Cosmetically, a predictable result is obtained due to the straight line of the ligature that causes the wound. It is a quick procedure for the physician to perform—once mastered.
No bandage is required, allowing easy monitoring for infection.
Healing occurs while the edges of the prepuce are secured in the ring, making skin bridges (where the foreskin's end heals to the glans' corona) unlikely.
Cosmetically, there will be little to no circumcision scar, though as usual with any circumcision, there will be a color change where the (formerly) inner and outer layers of foreskin are healed together.
Disadvantages
The ring must fall off before final healing can occur. Rarely, the tip of the glans may protrude through the ring and become swollen, trapping the ring in place. Blood transfusion risk 1 in 30,000 procedures (Wiswell).
One study of 2000 Plastibell circumcisions found a complication rate of 1.8%.[3]
The foreskin must first be slit and forced from the glans to allow entry for the plastic dome.
Furthermore, because convalescence depends on a (temporarily) affixed medical device, risks of infection or hemorrhage due to the bell slipping or otherwise failing are greater than a Gomco clamp or similar entirely-supervised circumcision.
There are several reports in the literature of urinary retention after circumcision with the Plastibell device.[4] Death has been reported.[5][6][7]
There also is a report of impetigo caused by Staphylococcus aureus when using the Plastibell.[8]
There have been multiple cases of children developing necrotizing fasciitis in their penis after being circumcised using the Plastibell device.[9][10]
There have been cases of necrosis of the glans penis following circumcision with the Plastibell device.[11]
"Non cutting"?
PlastiBell is often described to parents as a non-cutting method. However, a dorsal slit (cut) must often performed at the beginning of the installation to make it easier to install. Once installed, the PlastiBell cuts circulation to the foreskin, necrotizing the tissue, which will fall off in a few days (or it might be 'trimmed' after installing the PlastiBell). The result is the same: the amputation of a healthy, functional foreskin.
External links
References
- ↑
 Miller, RL; with Snyder DC [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Immediate circumcision of the newborn male. Am. J. Obstet. Gynecol.. 65(1): 1-11. PMID.
Miller, RL; with Snyder DC [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Immediate circumcision of the newborn male. Am. J. Obstet. Gynecol.. 65(1): 1-11. PMID.
- ↑
 Kariher, DH; with Smith TW [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Immediate circumcision of the newborn. Obstet Gynecol. 7(1): 50-3. PMID.
Kariher, DH; with Smith TW [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Immediate circumcision of the newborn. Obstet Gynecol. 7(1): 50-3. PMID.
- ↑ Izzidien Al-Samarrai A.Y., Mofti A. Crankson S. J The Use of Plastibell in Neonatal Circumcision. Review of 2000 cases. Surg. Gyne & Obst.167: 341-343, 1988
- ↑
 Ly, L; with Sankaran K [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Acute venous stasis and swelling of the lower abdomen and extremities in an infant after circumcision. CMAJ. 169(3): 216-7. PMID. Retrieved 23 April 2025.
Ly, L; with Sankaran K [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Acute venous stasis and swelling of the lower abdomen and extremities in an infant after circumcision. CMAJ. 169(3): 216-7. PMID. Retrieved 23 April 2025.
- ↑ Paediatrics & Child Health, Home
- ↑ http://www.austlii.edu.au/cgi-bin/sinodisp/au/cases/vic/VCAT/2010/1772.html?stem=0&synonyms=0&query=anaesthetic
- ↑
 Paediatric Death Review Committee: Office of the Chief Coroner of Ontario. Circumcision: A minor procedure?. Paediatrics & child health. 12(4): 311-2. PMID. PMC. Retrieved 25 April 2025.
Paediatric Death Review Committee: Office of the Chief Coroner of Ontario. Circumcision: A minor procedure?. Paediatrics & child health. 12(4): 311-2. PMID. PMC. Retrieved 25 April 2025.
- ↑
 Stranko, j; with ME Ryan, AM Bowman [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Impetigo in newborn infants associated with a plastic bell clamp circumcision. Pediatric infectious disease. 5(5): 597-9. PMID.
Stranko, j; with ME Ryan, AM Bowman [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Impetigo in newborn infants associated with a plastic bell clamp circumcision. Pediatric infectious disease. 5(5): 597-9. PMID.
- ↑
 Bliss, David P.; with Patrick J. Healey, John H.T. Waldhausen [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Necrotizing fasciitis after Plastibell circumcision. The Journal of Pediatrics. 131(3): 459-62. PMID. DOI.
Bliss, David P.; with Patrick J. Healey, John H.T. Waldhausen [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Necrotizing fasciitis after Plastibell circumcision. The Journal of Pediatrics. 131(3): 459-62. PMID. DOI.
- ↑
 Woodside, JR. Necrotizing fasciitis after neonatal circumcision. American journal of diseases of children. 134(3): 301-2. PMID.
Woodside, JR. Necrotizing fasciitis after neonatal circumcision. American journal of diseases of children. 134(3): 301-2. PMID.
- ↑
 Bode, C.O.; with S. Ikhisemojie, A.O. Ademuyiwa [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Penile injuries from proximal migration of the Plastibell circumcision ring. Journal of Pediatric Urology. 6(1): 23-7. PMID. DOI.
Bode, C.O.; with S. Ikhisemojie, A.O. Ademuyiwa [deprecated REFjournal parameter used: <coauthors> - please use <last2>, etc.]. Penile injuries from proximal migration of the Plastibell circumcision ring. Journal of Pediatric Urology. 6(1): 23-7. PMID. DOI.